Binge Eating Disorder (BED) is a prevalent yet often underdiagnosed condition in patients seeking obesity treatment. It is the most common eating disorder in US adults, occurring in approximately 3.5% of people.
Characterized by episodes of consuming large quantities of food, often accompanied by feelings of loss of control, BED affects approximately 30% of individuals seeking obesity treatment.
Clinicians play a critical role in recognizing, diagnosing, and treating BED, which requires a multi-faceted approach encompassing behavioral therapies, medication, and patient-centered communication. This document provides an overview of BED, its impact on obesity, and evidence-based strategies for effective management.
1. Recognizing and Diagnosing BED
Binge Eating Disorder is not simply overeating. It involves a psychological component where individuals feel an inability to control their eating and often experience shame, guilt, or distress afterward. This can lead to physical health complications, including type 2 diabetes, cardiovascular diseases, and high blood pressure, as well as mental health issues like depression and anxiety.
Key Indicators of BED:
- Loss of Control: Patients report feeling unable to stop eating, even when they are full.
- Rapid Eating: Individuals with BED tend to eat quickly, sometimes to the point of discomfort.
- Emotional Distress: After binge episodes, patients often feel guilty, ashamed, or distressed.
In a large study, the BEDS-7 algorithmic scheme yielded 100% sensitivity and 38.7% specificity in study participants.
Binge Eating Disorder Screener-7 (BEDS-7)
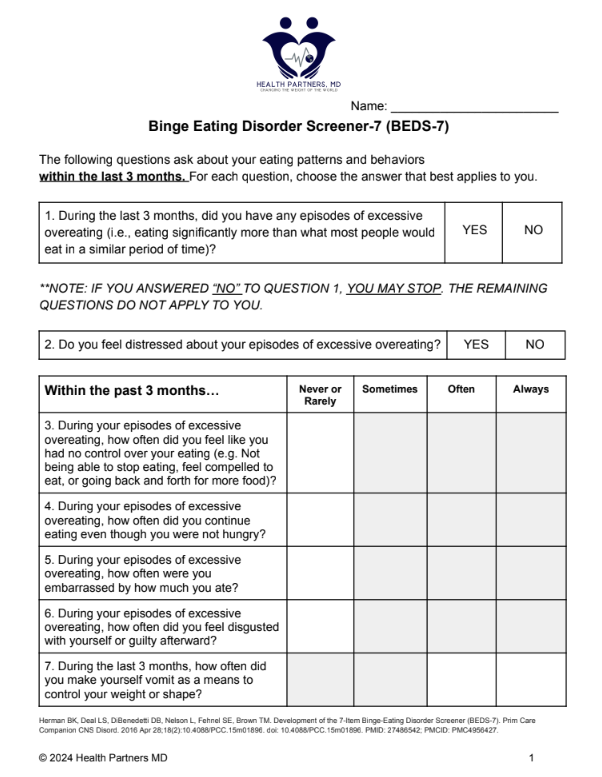
If the patient answers “NO” to question 1, there is no reason to proceed with the remainder of
the screener.
If the patient answers “YES” to question 1, continue to questions 2 through 7.
If the patient answers “YES” to question 2 AND checks one of the shaded boxes for all
questions 3 through 7, further screening should ensue.
According to the DSM-V, patients with BED must meet the following criteria:
| Criteria Set | Specific Definitions for Each Criterion |
| Criterion 1 | The binge eating occurs, on average, at least 2 days a week for 6 months (DSM-IV frequency and duration criteria) and at least 1 day a week for 3 months (DSM-5 frequency and duration criteria) |
| Criterion 2 | The binge eating occurs, on average, at least 2 days a week for 6 months (DSM-IV frequency and duration criteria)at least 1 day a week for 3 months (DSM-5 frequency and duration criteria) |
| Criterion 3 | Marked distress regarding binge eating is present. |
| Criterion 4 | DSM-IV does not include a BED severity grading scale. Applicable to DSM-5 only, BED severity is graded as follows: – Mild: 1 to 3 episodes per week – Moderate: 4 to 7 episodes per week – Severe: 8 to 13 episodes per week – Extreme: 14 or more episodes per week |
| Criterion 5 | The binge eating is not associated with the regular use of inappropriate compensatory behavior (e.g., purging, fasting, excessive exercise) and does not occur exclusively during the course of anorexia nervosa or bulimia nervosa. |
| Severity Grading | DSM-IV does not include a BED severity grading scale. Applicable to DSM-5 only, BED severity is graded as follows: – Mild: 1 to 3 episodes per week – Moderate: 4 to 7 episodes per week – Severe: 8 to 13 episodes per week – Extreme: 14 or more episodes per week |
2. Understanding the Psychological and Emotional Roots of BED
The psychological underpinnings of BED often involve emotional triggers such as stress, boredom, or past trauma. For some patients, food becomes a coping mechanism, providing temporary relief from emotional pain but ultimately leading to a cycle of negative feelings and continued binge eating episodes. Additionally, individuals with BED may have experienced weight bias, which exacerbates feelings of low self-esteem and body dissatisfaction.
Behavioral and Emotional Contributors:
- Emotional Eating: Many individuals with BED use food as a way to cope with emotional stressors, which can be triggered by personal, social, or environmental factors.
- Body Image Issues: Weight stigma and societal pressures around body image can contribute to the development and persistence of BED.
- Cross-Addiction: Some patients may substitute one addictive behavior for another; for example, after bariatric surgery, they might turn to alcohol or other substances if they previously used food for emotional comfort.
3. Evidence-Based Treatments for BED
Effective treatment of BED includes a combination of psychological counseling, medication, and lifestyle interventions. Cognitive Behavioral Therapy (CBT) is the most widely recommended approach, focusing on helping patients identify and change negative thought patterns that lead to binge eating. Additionally, some patients may benefit from medication to help reduce episodes of binge eating. Obesity treatment is not a substitute for BED treatment. Treating excess weight does not treat BED. Similarly, bariatric surgery is not a cure for binge eating disorder and patients typically have worse outcomes after bariatric surgery if binge eating disorder is not addressed first.
Treatment Strategies:
- Cognitive Behavioral Therapy (CBT): CBT helps patients identify emotional triggers for binge eating and develop healthier coping mechanisms. This therapy has shown to be effective in reducing the frequency of binge episodes.
- Medications: The FDA-approved medication Vyvanse (lisdexamfetamine) can reduce binge episodes in patients with moderate to severe BED. Other medications, such as selective serotonin reuptake inhibitors (SSRIs), can also help by addressing underlying depression or anxiety.
- Supportive Counseling: Counseling that addresses body image issues and weight stigma can help patients build self-esteem and create healthier relationships with food.
4. Creating a Supportive, Inclusive Environment for Patients with BED
To encourage patients with BED to seek and adhere to treatment, medical offices should create a supportive, stigma-free environment. This includes using patient-first language, providing educational materials that address BED specifically, and training staff to handle sensitive conversations about weight and eating habits with empathy and respect.
Best Practices:
- Patient-First Language: Use terms that prioritize the person, such as “patient with BED” rather than “binge eater,” to reduce stigma.
- Inclusive Resources: Stock waiting areas with reading materials that reflect body positivity and wellness beyond weight loss, reducing the focus on appearance.
- Ongoing Education: Training staff to recognize signs of BED and handle discussions about eating habits without judgment helps create a safer, more supportive environment for patients.
Binge Eating Disorder is a serious mental health condition that impacts physical and emotional well-being. By identifying, diagnosing, and treating BED with evidence-based strategies, clinicians can support patients in achieving improved health outcomes. For practices that lack the resources to provide specialized care for BED, referring patients to a team with expertise in obesity and eating disorder treatment is a practical approach to ensure comprehensive, compassionate care.

